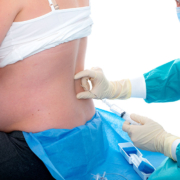
Using Epidural Anesthesia During Labor: Benefits and Risks
Using Epidural Anesthesia During Labor: Benefits and Risks
Epidural anesthesia is a regional anesthesia that blocks pain in a specific part of the body, making it the most preferred method of pain relief during labor. Women request it by name more than any other pain relief method. The primary aim of an epidural is to provide analgesia, or pain relief, rather than total anesthesia, which results in a complete absence of sensation. Epidurals work by blocking nerve impulses from the lower spinal segments, and over 50% of women in hospitals opt for this type of anesthesia during childbirth.
Types of epidurals?
Regular Epidural: Once the catheter is positioned, a mix of a narcotic and an anesthetic is delivered either through a pump or by periodic injections into the epidural space. To supplement the higher doses of anesthetic required, narcotics such as fentanyl or morphine are used.
Combined Spinal-Epidural (CSE) or “Walking Epidural”: An initial dose of narcotic, anesthetic, or both is injected into the intrathecal space, located just beneath the outermost membrane covering the spinal cord and deeper than the epidural space. After this, the anesthesiologist retracts the needle to the epidural space, inserts a catheter through the needle, removes the needle, and leaves the catheter in place for continuous pain relief. This method offers more mobility in bed and the ability to change positions with assistance. You can request additional epidural pain relief through the catheter if needed. Generally, CSE provides pain relief for 4-8 hours.
Benefits of Epidurals During Delivery
- Potential for a painless delivery.
- Allows rest during prolonged labor.
- Can enhance the childbirth experience by reducing discomfort.
- Essential for cesarean delivery, enabling you to remain awake and providing effective pain relief during recovery.
Risks of Epidurals During Delivery
- Low blood pressure: Approximately 14% of women experience a drop in blood pressure with an epidural, which is typically not harmful. Healthcare professionals will monitor your blood pressure closely, administering fluids and medication as needed to maintain it.
- Loss of bladder control: The epidural may numb the nerves around your bladder, making it difficult to sense when it’s full. A catheter may be inserted to manage urination until the epidural’s effects wear off.
- Nausea and vomiting: Opioid pain relievers used in epidurals can cause nausea and vomiting as side effects.
- Fever: About 23% of women with an epidural develop a fever, compared to 7% without one. The cause of the temperature increase is unclear.
- Permanent nerve damage: Although rare, there’s a slight risk of permanent sensory or motor loss in the legs.
Other complications
Very rare complications include seizures, severe breathing difficulties, and in extremely rare cases, death.
When is an epidural NOT an option?
- If taking certain medications
- With heavy bleeding or low platelet counts
- In the presence of an infection on or near the back
- If experiencing hemorrhage or shock
- Labor is progressing too rapidly
- The epidural space cannot be located
- Inadequate dilation (less than 4 cm)
- Abnormal blood work
Considerations and Restrictions:
Discuss the benefits and risks of epidural anesthesia with your anesthetist to make an informed decision. While epidurals offer significant pain relief, they come with potential side effects. Your decision should be based on your personal pain tolerance and preferences.
Disclaimer
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. The purpose of this website is to promote broad consumer understanding and knowledge of various health topics. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition or treatment before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
References:
https://www.healthline.com/health/pregnancy/natural-birth-vs-epidural
https://www.healthline.com/health/pregnancy/pain-risks-epidurals