Gestational Diabetes and Pregnancy: What you need to know
Gestational diabetes mellitus or GDM is one of the most common diet-related complications during pregnancy. It only happens during pregnancy. It means you have high blood sugar levels, but those levels were normal before you were pregnant.
In gestation, the placenta produces hormones that help the baby to grow and develop. These hormones also block the action of the insulin, which is the hormone that helps to keep glucose (or blood sugar) at normal levels. This is called insulin resistance. Because of this insulin resistance, the need for insulin in pregnancy is 2 or 3 times higher than normal. If the body is unable to produce this much insulin, gestational diabetes develops.
If you have it, you can still have a healthy baby with help from your doctor and by doing simple things to manage your blood sugar, also called blood glucose.
It is most commonly diagnosed around the third trimester (usually around the 24th to 28th week of pregnancy) and in most of the cases goes away once the baby is born. Gestational diabetes makes you more likely to develop type 2 diabetes, but it won’t definitely happen.
WHO ARE AT GREATER RISK?
It affects between 2% and 10% of pregnancies each year. Women who are at greater risk of developing gestational diabetes are:
- Mothers who are over 25 years of age
- Having a family history of type 2 diabetes
- Were overweight before you got pregnant
- Women from certain ethnic backgrounds including Vietnamese, Chinese, middle eastern, Polynesian or Melanesian.
- Women who have had gestational diabetes
- Women who have had large babies or obstetric complications
- Have given birth to a baby that was stillborn or had certain birth defects
- A woman who has had a polycystic ovarian syndrome
Gestational Diabetes Symptoms
Women with gestational diabetes usually have no symptoms. Most learn they have it during routine pregnancy screening tests.
Rarely, especially if the gestational diabetes is out of control, you may notice: 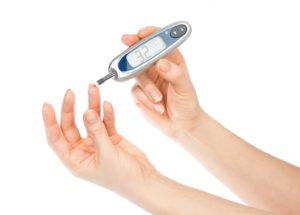
- Feeling more thirsty
- Feeling more hungry and eating more
- A need to pee more
Gestational Diabetes Treatment
To treat your gestational diabetes, your doctor will ask you to:
- Check your blood sugar levels four or more times a day.
- Do urine tests that check for ketones, which mean that your diabetes is not under control
- A balanced diet is key to properly managing gestational diabetes. In particular, women with gestational diabetes should pay special attention to their carbohydrate, protein, and fat intake.
- Eat a healthy diet that’s in line with your doctor’s recommendations
- Make exercise a habit
Your doctor will track how much weight you gain and let you know if you need to take insulin or other medicine for your gestational diabetes.
Why Is Managing Blood Sugar Especially Important for Pregnant Women With Gestational Diabetes? 
Most women who develop diabetes during pregnancy go on to have a healthy baby. Dietary changes and exercise may be enough to keep blood sugar (glucose) levels under control, though sometimes you may also need to take medication.
But untreated gestational diabetes can cause serious problems. If blood sugar levels remain elevated, too much glucose ends up in the baby’s blood. When that happens, the baby’s pancreas needs to produce more insulin to process the extra sugar.
Too much blood sugar and insulin can make a baby put on extra weight, which is stored as fat. This can make the baby grow very large (macrosomia).
Also, high blood sugar levels during pregnancy and labor increase the risk of a baby developing low blood sugar (hypoglycemia) after delivery. That’s because the baby’s body produces extra insulin in response to the mother’s excess glucose. Insulin lowers the amount of sugar in the blood.
The signs and symptoms of hypoglycemia in an infant include:
- jitteriness
- weak or high-pitched cry
- floppiness
- lethargy or sleepiness
- breathing problems
- skin that looks blue
- trouble feeding
- eye rolling
- Seizures
A baby may also be at higher risk for breathing problems at birth, especially if blood sugar levels aren’t well controlled or the baby is delivered early. (If you have gestational diabetes, your baby’s lungs tend to mature a bit later). The risk of newborn jaundice is higher too.
If your blood sugar control is especially poor, the baby’s heart function could be affected as well, which can contribute to breathing problems. Gestational diabetes sometimes thickens a baby’s heart muscle (hypertrophic cardiomyopathy), causing the baby to breathe rapidly and not be able to get enough oxygen from her blood.
Can gestational diabetes be prevented?
It’s not possible to prevent gestational diabetes entirely. However, adopting healthy habits can reduce your chances of developing the condition. If you’re pregnant and have one of the risk factors for gestational diabetes, try to eat a healthy diet and get regular exercise. Even light activity, such as walking, may be beneficial.
If you’re planning to become pregnant in the near future and you’re overweight, one of the best things you can do is work with your doctor to lose weight. Even losing a small amount of weight can help you reduce your risk of gestational diabetes.
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. The purpose of this website is to promote broad consumer understanding and knowledge of various health topics. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.



Leave a Reply
Want to join the discussion?Feel free to contribute!