Introduction to Physiological Changes in Pregnancy
Pregnancy induces physiological changes to nurture the developing fetus and prepare the mother for labor. These changes affect biochemical values and can mimic symptoms of medical conditions. Distinguishing between normal physiological changes and disease pathology is crucial.
Understanding Physiological Changes
Pregnancy impacts all maternal organ systems, with most changes reverting post-delivery. These adjustments occur due to hormonal shifts, increased blood volume, weight gain, and the growing fetus. Affected systems include the musculoskeletal, endocrine, reproductive, cardiovascular, respiratory, nervous, urinary, gastrointestinal, and immune systems. Skin and breasts also undergo changes. A full-term pregnancy lasts 39-40 weeks, with pre-term birth defined as delivery before 37 weeks. The duration of human pregnancies can naturally vary.
The Purpose of Pregnancy
The primary goal of pregnancy is fetal growth and development. Changes in the mother’s body support this growth and the development of the placenta. This sustains the pregnancy and nourishes the fetus.
Risks of Hypercoagulability
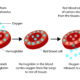
Pregnant women face an increased risk of blood clots and embolisms, making them 4-5 times more likely to develop clots than non-pregnant women. Hypercoagulability, which likely evolved to minimize hemorrhage risks during miscarriage or childbirth, increases the likelihood of conditions like deep vein thrombosis and pulmonary embolism. Hemorrhage remains a leading cause of maternal death in third-world countries, while in the United States, it accounted for 11.4% of all pregnancy-related deaths between 2011-2013.
Factors Increasing Clot Risks
Several factors elevate clot risks during pregnancy. These include heightened plasma levels of pro-coagulation factors and changes in platelet reactivity. The enlarging uterus can compress the vena cava, causing blood stasis. Risk factors for clots include thrombophilia, cesarean section, and preeclampsia. Clots typically form in the left leg or the left iliac/femoral venous system. Cases of May-Thurner Syndrome, where the right common iliac artery compresses the left common iliac vein, have also been reported.
Physiological Changes in Multifetal Pregnancies
Physiological changes are more pronounced in multifetal pregnancies. These adaptations help the mother support the uterus and fetus, and manage labor and the postpartum period. Understanding these changes is vital, especially if the pregnant woman requires surgery.
Disclaimer
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. The purpose of this website is to promote broad consumer understanding and knowledge of various health topics. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.

 ToronTek
ToronTek